Estimated read time: 5-6 minutes
This archived news story is available only for your personal, non-commercial use. Information in the story may be outdated or superseded by additional information. Reading or replaying the story in its archived form does not constitute a republication of the story.
SALT LAKE CITY — An audit of Utah’s COVID-19 testing system came up with five recommendations for state leaders and health officials to improve coronavirus testing delay times, including working with labs to figure out ways to speed up the results process, create a standard turnaround time for results and to make turnaround times more transparent.
Those suggestions came after it found “inconsistencies in messaging surrounding test turnaround time” that ranged from 24 to 72 hours and that testing labs had wide-ranging result times that lasted as long as almost four days — more than twice the state average.
It also found providers weren’t required to report the time from when they received a COVID-19 test result to when they informed a patient of the result. That finding clouded an understanding of how long it actually takes Utahns to receive COVID-19 test results, which could have dire effects in the state’s fight to control the coronavirus.
The Office of the Legislative Auditor General completed the audit Tuesday. It was completed as state health officials are trying to determine what’s causing a recent decline in COVID-19 testing.
“We fully support their recommendations and publishing testing turnaround times to increase transparency. We are confident the Utah Department of Health and the Governor's Office of Management and Budget will collaborate and improve the process,” Utah Senate President J. Stuart Adams and House Speaker Brad Wilson said in a prepared statement together.
According to the report, the average test in Utah takes 38 hours, or 1.6 days, from swab to a result to be sent to a provider, but that number does range depending on the lab. For example, in a review of data from six labs from June 26 to July 16, it found it can take anywhere from 1.3 to 3.7 days for a result. Two of the labs that averaged results in 1 ½ days accounted for more than half of the test results.
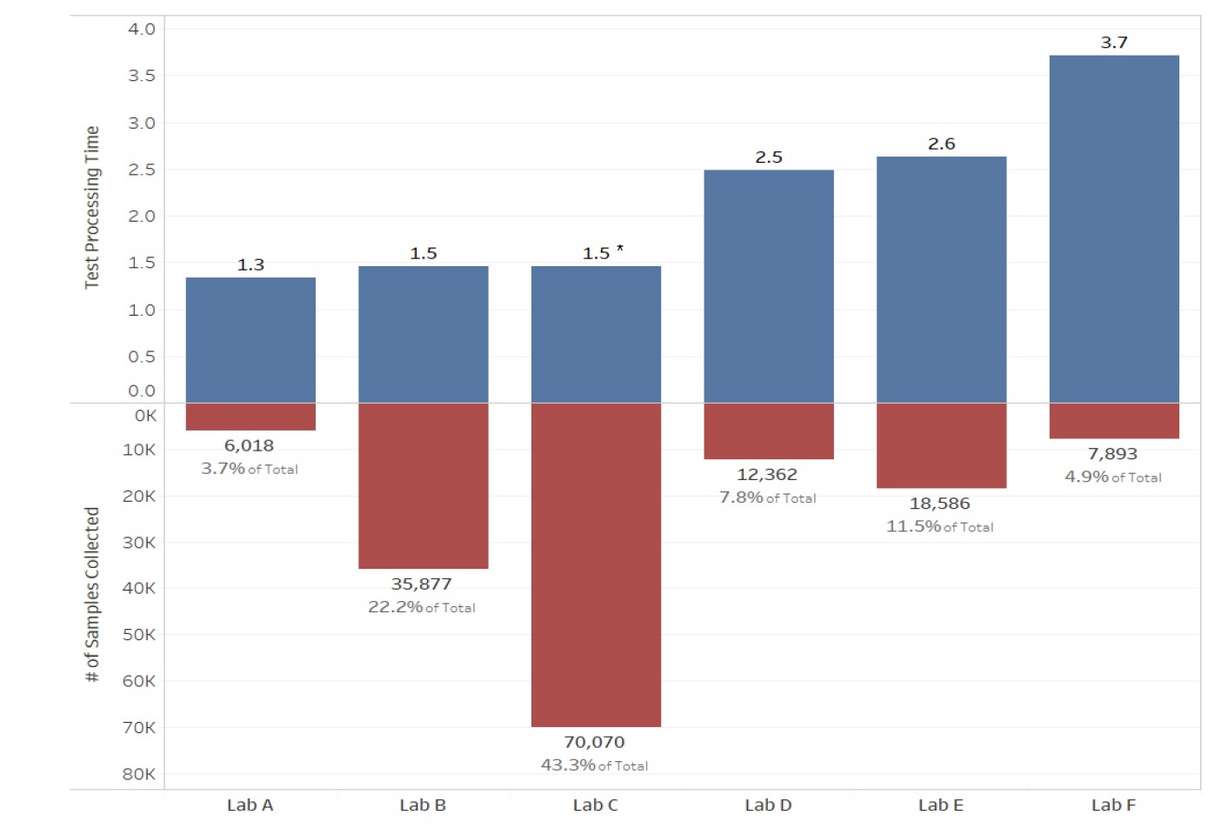
Officials said this variation in time could be related to one lab having higher demand than another, but the study didn’t account for that variable. The labs weren’t identified in the report, but the lab with the longest delay time slipped from an average of 2.3 days from April 16 to June 25 to 3.7 days during the defined 21-day stretch beginning June 26.
Experts told auditors that tests outside of the Wasatch Front typically do take longer to process because it takes extra time to transport the samples. Other factors like strained resources and staffing can come into play, as well.
Once those results are in, they are given to a provider and it’s up to that provider to contact test results to a patient. The report stated that the “most critical measure” is the time a patient gets swabbed to the time they receive results, which isn’t known since the final part of the process wasn’t tracked.
Testing speed is an important aspect of the testing process. Citing a Utah Department of Health representative and a member of Utah’s COVID-19 Unified Command Team, the report noted that delays in test results can lead to further spread of COVID-19 if the carrier doesn’t take precautions, makes contact tracing “exponentially more difficult” because there is a longer amount of time to track a carrier’s whereabouts, and possibly lead to a lost opportunity for a carrier to get early medical care. In addition, it could lead to economic losses from someone unable to work as they wait for a result to come in.
As a result of their findings, the report recommended that the Utah Governor’s Office and department of health work together to create a goal for the time a test is conducted to the time a result is discovered and from that time to when the patient is informed. It was also recommended that a commission be created by the health department to look into the possibility of collecting data on the time a test result comes in to the time a result is given to the patient.
It also recommended the health department publish test processing times based on labs and their location in the state; that the health department work with labs and providers on ways to reduce test turnaround times and that the health department look into the possibility of creating a system to move test samples from backlogged labs to labs with more capacity.
Rich Saunders, who was appointed the interim executive director of the state health department last week, responded to the report in a letter provided by the state. In it, he wrote that the department agreed with the recommendations and set up a timeline for them to be implemented by the end of the month.
The state health department’s Testing Coordination Council will look to see if it’s feasible to collect the complete turnaround times, including the time from a provider getting a result to the time they inform a patient. The department will also work with the state legislature to make more of the processing times available on the state’s COVID-19 website, Saunders wrote.
The department is also working with the Governor’s Office and State Legislature to discuss a turnaround goal for the Utah Public Health Laboratory; Saunders wrote the department has worked with labs in Utah from the beginning of the pandemic on improving turnaround times, and was discussing a “partnership with a university to see if some testing can be done at one of their labs” as a possible solution to backlogged labs.
Kristen Cox, executive director of the Governor’s Office of Management and Budget, also agreed with the findings, calling testing cycle times “often the longest part of the process.”
“Because the state does not have direct oversight over other labs, it welcomes sharing best practices across all of the labs to improve processing while also sharing information on new and promising testing modalities,” she wrote.









