Estimated read time: 9-10 minutes
This archived news story is available only for your personal, non-commercial use. Information in the story may be outdated or superseded by additional information. Reading or replaying the story in its archived form does not constitute a republication of the story.
SALT LAKE CITY — Utah’s COVID-19 case totals have doubled in less than a month. State health officials fear if the number of cases continues to grow at this rapid rate, patients are going to jam up intensive care units in some Utah hospitals as early as next month.
That’s why leaders of Utah’s four largest health care systems and the Utah Hospital Association launched a new public awareness initiative Tuesday aimed at normalizing mask wearing in an effort to get Utahns to wear masks. The campaign, "#MaskUpUtah," will include advertisements across many visible platforms throughout the summer. They hope more regular mask use will slow down the spread of COVID-19 and avoid a potential hospital crisis.

"Masking is not about you; masking is about everyone around you," said Dr. Michael Baumann, chief medical officer for MountainStar Healthcare, during a virtual press briefing with reporters Tuesday. "This is to prevent the spread of potential COVID from you to someone else. That’s the key to remember. … This is a health care issue; this should not be a political issue. Masking is about basic health and preventing the spread of disease to family, friends and even people you don’t know."
Their message comes as some cities and states have started requiring masks to be worn in public. Salt Lake County Mayor Jenny Wilson and Salt Lake City Mayor Erin Mendenhall both tweeted Tuesday urging Gov. Gary Herbert to make wearing masks mandatory. The Utah Governor's Office issued a prepared statement this week saying that they will continue to be recommended.
"The Governor continues to be a strong champion for regular wearing a face covering in public when physical distancing is not possible," the statement reads, in part. "He wears a mask each day to all of his meetings and expects it of those who meet with him. We expect all Utahns to follow the common sense built into our current guidelines."
The organizations also rolled out the campaign a little over an hour after Utah Department of Health officials announced 394 new cases had been reported in the state. In all, 18,300 cases have been reported in the state since March 6 — 9,779 of those after Memorial Day.
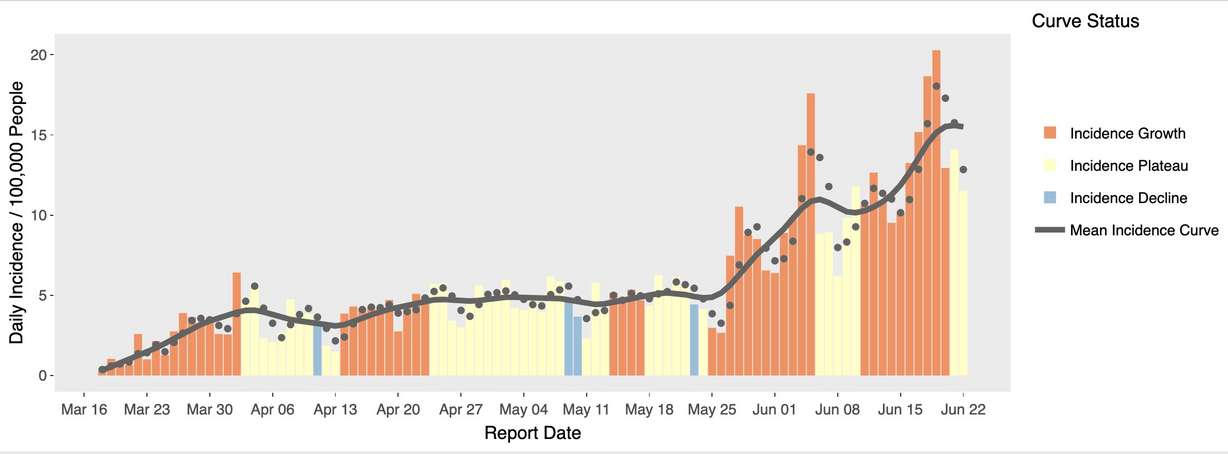
That’s led to a rise in both daily and overall hospitalizations, too. There were 166 Utahns still hospitalized as of Tuesday. That’s compared to 95 Utahns who were hospitalized on Memorial Day. There have been 534 total COVID-19 hospitalizations since the May 25 holiday, as well. That’s a 77% increase in Utah’s total hospitalizations over the span of nearly one month.
As of Tuesday, 62% of all ICU beds in the state were occupied for all reasons, including COVID-19. Non-ICU beds were 45% occupied. But in a brief that was made public Monday, Dr. Angela Dunn, the state’s epidemiologist, warned state leaders that hospitals may soon reach a critical state if COVID-19 continues to spread at the rate it has over the past few weeks. Her memo, which was dated Friday, said that if Utah didn’t return back to a seven-day average of 200 cases per day by July 1, then the state should move back to orange on its reopening scale and mandate face coverings either by government or business enforcement.
"We need to be clear with (the) public about why decisions are being made lessening restrictions — economic, not health. Be clear about health risk," she wrote in the brief. If those suggestions aren't reasonable, "be clear about how these decisions are made and who makes them," she said. "This will better equip the public to make informed decisions about how to protect themselves and their health."
Dr. Mark Briesacher, chief physician executive for Intermountain Healthcare, said his hospitals' predictive models show they may run out of "conventional ICU" space at some hospitals in the next 4-6 weeks. The health care system does have plans in place for what happens once those beds are filled, but it’s a scenario they don’t want to use if they don’t have to.
Dr. Arlen Jarrett, chief medical officer for Steward Health Care, said his company’s hospitals across Utah were at about half-capacity and have worked to secure supply chains over the past few months to prepare for future issues. That said, they’ve noticed an uptick over the past few weeks.
"The good news is that, for whatever variety of reasons in Utah, the people who have died from the COVID disease is actually a pretty low rate," he said, adding that the state’s mortality rate remains lowest in the country even as cases spike. That said, he finds the current trend to be troubling.
"We can’t keep going the direction we’re going," he continued, saying that 60% of cases are spread from household contact and almost all were spread through someone in either a work or social setting with someone they know. "We know that we’ve got to do something out there while we’re in society to protect our families. We’ve shown we can do this before with some really drastic lockdown measures, but I feel quite certain we can do this — and I’m optimistic that we can do this — without those lockdown measures if we’d just take our responsibility and practice (health guidelines)."
How masks play into the equation
The easiest way to slow down hospitalizations is to slow down case counts. Even though Tuesday’s numbers indicate 6.7% of all reported cases have led to hospitalizations, Dunn pointed out that there’s usually at least a week in lag time between a new case turning into a possible hospitalization. Her projections were based on hospitalizations remaining close to 8% as they have been for the past few months.
All types of masks can play into helping reduce the spread, Utah’s health care leaders and doctors say. Even though death from COVID-19 might be rare, especially for younger individuals with no pre-existing health conditions, someone could still spread the disease to another person who might get a severe case.
This is a health care issue; this should not be a political issue. Masking is about basic health and preventing the spread of disease to family, friends and even people you don’t know.
–Dr. Michael Baumann, chief medical officer for MountainStar Healthcare
While medical-grade masks may reduce upwards of 95% of particles that a wearer inhales, health officials say the largest role cloth masks and other coverings have is preventing droplets from coughs and sneezes. If everyone outside their home, especially those who are in situations within 6 feet of each other, has a properly-worn mask, that reduces the amount of droplets released into the air that may contain COVID-19. It’s important, they say, because someone may unknowingly spread it in some cases.
"Since COVID-19 can be spread or individuals can be infectious without our knowing it, we can have mild symptoms or be asymptomatic (and spread the disease)," said Dr. Jeanmarie Mayer, an epidemiologist for University of Utah Health Care. "It’s most critical that we’re wearing our mask when we’re around other individuals."
Dr. Eddie Stenehjem, an infectious diseases physician for Intermountain Healthcare, referred to a recent news story when two hair salon employees in Missouri tested positive for COVID-19, potentially infecting 146 other people. The salon required both employees and customers to wear masks. The local health department where it happened reported on June 8 that none of the 146 co-workers or customers were infected.
"It really just shows how beneficial a mask can be when worn in social environments like that," he said. "We’re going to see more and more examples of this come out in the media as our medical literature catches up with all of this. It’s absolutely clear that wearing a mask is preventative and will definitely save lives."
Health care professionals also pushed back narratives brought up online about people who refuse to wear masks, citing a multitude of reasons. Those include people who say they won’t because they have a breathing issue or even those who claim carbon dioxide buildup poses another health risk.
Related:
Decades of evidence shows that masks are safe from carbon dioxide issues, said Dr. Jeremy Voros, emergency medicine physician for Intermountain Healthcare. Health officials also said those who have severe breathing problems likely were already wearing a mask or some sort of protective material. Mayer added that there may have also been mixed messages about mask effectiveness early on and that may have also impacted opinion.
There are also different numbers as to how effective masks are regarding protecting droplets or inhaling droplets, Baumann acknowledged. He credited the problem to the disease spreading much quicker than researchers have time to finalize studies. He pointed to a British Medical Journal paper published in 2003 that jokingly asked if it was necessary to study if parachutes were needed when jumping out of an airplane.
"We don’t necessarily have all the data we need around masking but this is really a common sense issue," Baumann said. "We need to be doing what we need with masking to prevent spread. We would like more data, but what we don’t have is the time to wait for that data. This is very common sense. We need to be doing it now for the protection of others around us."
The ‘Mask Up’ message
Of course, it’s not just about masks. People should still practice social distancing as much as possible, practice good hand hygiene at all times, and stay at home when they aren’t feeling well. Masks are an additional tool in a very short list of ways to combat the coronavirus at this point, experts say.
That’s where the new campaign "#MaskUpUtah," comes into play. There will be billboards and media ads; Greg Bell, president and CEO of the Utah Hospital Association, said there will be a push to get employers to spread this message too as he unveiled mockups of the ad campaign.
"This has to be a nongovernmental initiative," he said, before he placed a medical mask over his face and pledging to "mask up" for his family. "When the government gets involved, it gets political. This is not a political issue. We can do this as a community. If we want to keep our economy open, we need to do this."
Other health experts pledged to "mask up" for grocery store employees and other workers at essential businesses, for friends and for medical colleagues. Considering the recent uptick began shortly after Memorial Day, they hope the message spreads quickly before the next holiday, July 4.
"Wearing the mask is clearly the key thing for us all to do," Jarrett said. "When we can’t keep more than 6 feet away from each other, we need to be wearing a mask so that we don’t spread this disease. … Sure, some masks might be better than other masks are at preventing spread, but they’re all good."










