Estimated read time: 5-6 minutes
This archived news story is available only for your personal, non-commercial use. Information in the story may be outdated or superseded by additional information. Reading or replaying the story in its archived form does not constitute a republication of the story.
Sean Johnson was camping at Duck Creek Village in southern Utah, when he lay down to sleep on the cot he'd recently purchased. That 2013 summer, six-foot-five Sean weighed 650 pounds and the cot was supposed to support 700 pounds of body weight. Instead it broke and he burst into tears.
"Is this life worth living right now?" he asked himself. His answer was no. He told his wife, "For the first time ever, I can tell you I'm not happy with who I am and I don't know how to change it."
The then-30-year-old had struggled with his weight all his life, but this was the breaking point. His family doctor told him his weight wasn't only a physical issue connected to exercise and diet, but also a mental one. Sean had been sexually abused as a child and that devastating trauma—and the shame, guilt and fear it had bred—had significantly contributed to his weight gain. "I was stuck in survival mode. I wasn't thinking about my future, just that I have to live."
His doctor placed Sean's fate in his own hands. "You're the captain of your life," he told him. "No one is going to do this for you. It's your decision."
Through therapy, Sean came to understand how his childhood trauma had impacted his life. But while he was able to address his trauma-related behavioral issues, the abuse he'd subjected his stomach to was another matter.
He spent months researching Mexican medical tours and weight loss clinics, before deciding, he says, that University of Utah Health's Comprehensive Weight Management Program was the best in the western region.
Juliana Simonetti, MD, co-director of the program, first encountered obesity working at a community care center in Boston during her residency. Every patient she saw had chronic diseases: pre-diabetes, high cholesterol, blood pressure and weight issues. Patients from lower socio-economic backgrounds were desperate to address their weight issues, spending much-needed money on over-the-counter diet pills that weren't FDA approved. With little training for doctors to treat patients for obesity, Simonetti says, "Instead of addressing the root causes of weight gain, I felt we were band-aiding."
One answer is medication, which can be key to addressing underlying physiological issues that make it so hard to lose weight, along with behavioral health approaches to addressing psychological issues related to obesity.
The comprehensive weight management program, Simonetti says, seeks to bring innovative approaches to obesity medicine. These include helping patients at different stages of their weight loss journey through low-impact exercise classes, group medical visits, mindfulness-based stress-reduction courses, behavior health referrals and helping patients find cheaper healthier food options and cooking classes. It is also one of very few programs in the country that brings together different specialists to help patients lose weight while treating the complications related to obesity and excess weight.
The key point is, "There's no magic pill," Simonetti says. "What we do is address the underlying issues, and suppress appetite and cravings."
Eric Volckmann, MD, is the director of U of U Health's Comprehensive Weight Management Program. He initially recommended Sean have a gastric bypass, but after further review, they decided on a gastric sleeve. "It's not as considerable on the weight-loss side," Sean says. "I knew it would be a longer, slower journey for me, but I wanted to remain active and a gastric bypass wouldn't permit that."
Sean lost 70 pounds pre-surgery, drinking protein shakes for breakfast, eating cottage cheese and sugar-free drinks. He had to re-teach his body before surgery, doing stretching and yoga and reading self-help books that emphasized realistic expectations. "You only get upset if you have expectations that aren't met," Sean says.
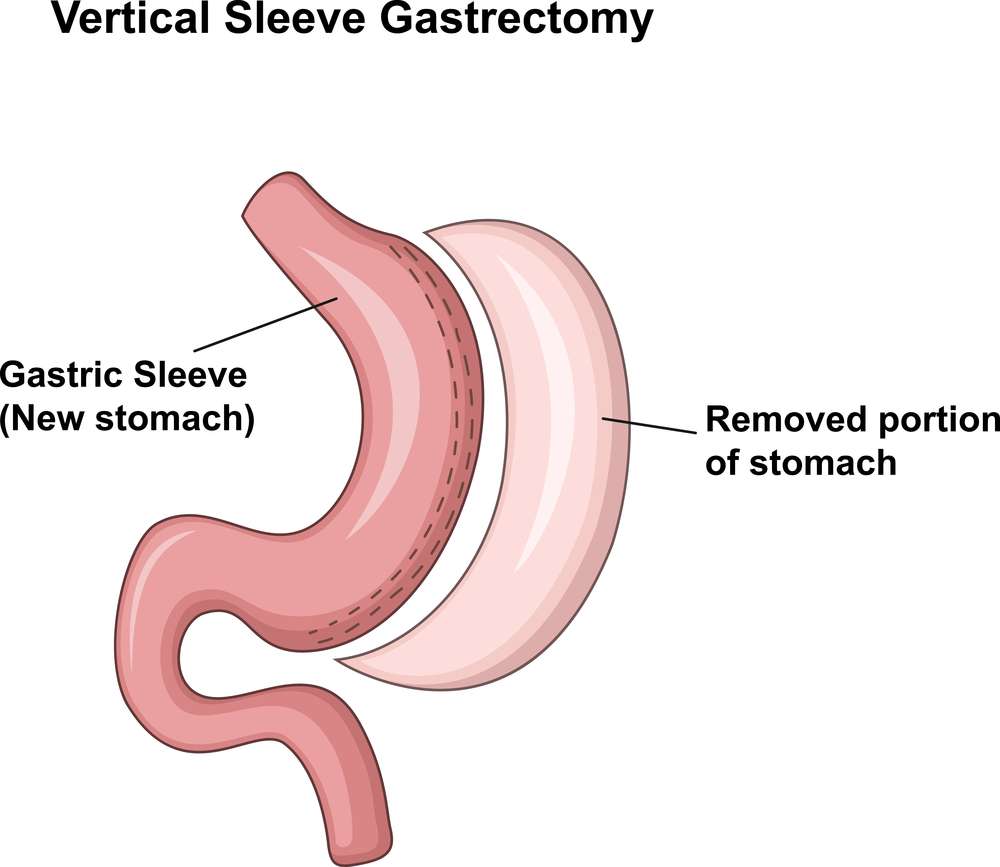
The gastric sleeve operation, which Sean had in May 2018, removed 90 percent of his stomach which Volckmann then stapled shut into a banana shape somewhere between the size of a golf ball and a tennis ball. "What's nice is you don't feel hungry; you eat a little food and you don't feel like you're starving," Sean says.
"A lot of people think it's an easy way out, but it's totally not." he says. "It's not a solution or a quick fix. It's very much just a tool to help. I've abused my body to a point where the gym isn't the only solution. I need other tools to help me."
He had to be on liquids for three weeks after the operation, before transitioning to soft food. "I got to a point I needed meat so badly, I blended up breadless chicken nuggets into a broth. And it wasn't bad." His wife was horrified, he says with a laugh.
By the end of 2019, Sean had dropped to 418 pounds. When the pandemic hit, he resolved that if he couldn't continue working on his weight loss with gym workouts, he could at least maintain. "I decided I would hunker down and just get through it, just chill." Even so by the start of the next year he had still managed to lose weight. By December 2020, he had lost another 28 pounds, coming in at 390 pounds, and now aims to lose 100 pounds more.
While program staff praise him for how determined he was to be the captain of his own weight-loss journey, Sean in turn is grateful to the U's program staff for all their support. "It's one of the best things I have ever done," he says.









