Estimated read time: 4-5 minutes
This archived news story is available only for your personal, non-commercial use. Information in the story may be outdated or superseded by additional information. Reading or replaying the story in its archived form does not constitute a republication of the story.
SALT LAKE CITY — The number of Utahns with antibodies from the novel coronavirus is lower than researchers expected, indicating we have “a highly susceptible population.”
“There are a lot of people who haven’t had this yet ... they’re all at risk of getting the infection,” said Steve Alder, professor of Family and Preventive Medicine at the University of Utah.
“The efforts to date have been pretty good, we’ve done a good job of managing disease and keeping infections low,” he said. “If we let our guard down, all of those gains could erode very quickly.”
The date he’s speaking of is actually three weeks ago, June 10 to be exact.
It was before the continued spike in cases throughout Utah, and the end of the first phase of the Utah Health and Economic Recovery Outreach project, for which Alder serves as director of field operations.
The HERO project is a collaboration between the U.’s David Eccles School of Business, University of Utah Health, Study Design and Biostatistical Core of the Center for Clinical and Translational Science, the Governor’s Office of Management and Budget, and the Hope Corps, to better understand how SARS-CoV-2 is really impacting the state of Utah.
And things aren’t looking good, they found.
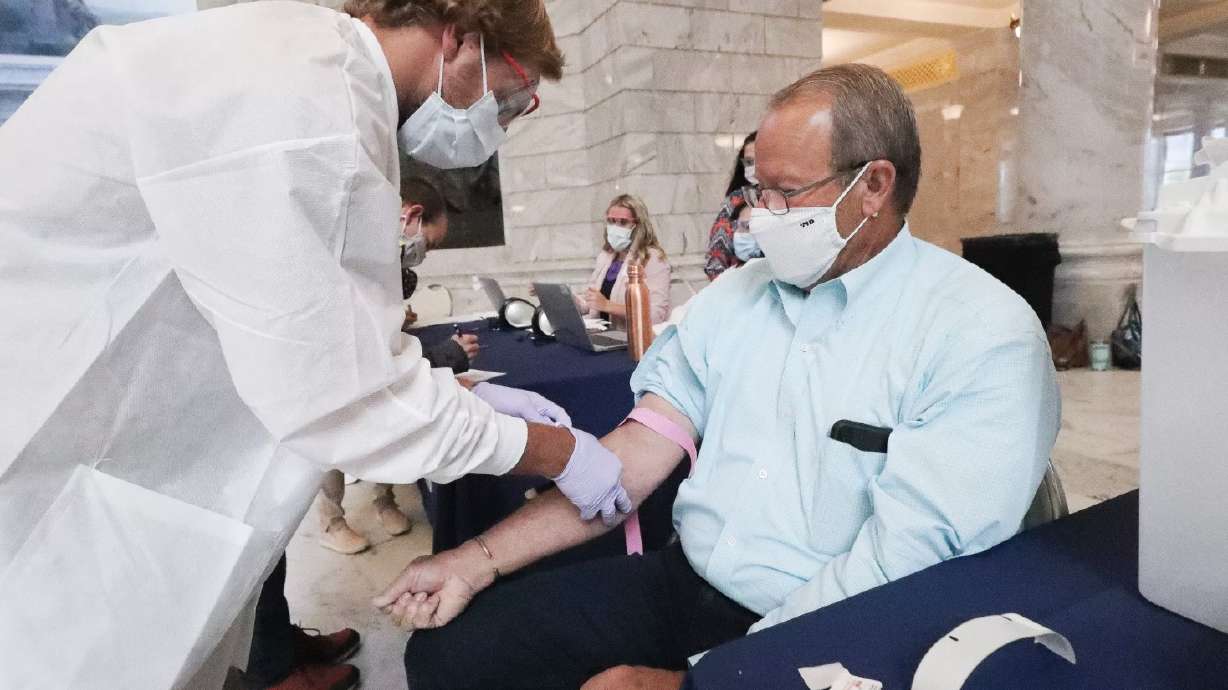
From May 4 to June 10, field workers collected antibody samples from 8,500 randomly selected Utahns, age 12 and older, from Davis, Salt Lake, Summit and Utah counties. The results, Alder said, were a bit surprising and the number of people who have been infected with the virus is “lower than anticipated.”
While officials with the U.S. Centers for Disease Control and Prevention have said there may be as many as 10 undetected cases of COVID-19 for every one case that is detected, that is not the case in Utah.
Study results show that for every case detected so far in Utah, there are probably about 2.4 additional cases that have gone undetected.
Related:
“The downside of that is that we have a highly susceptible population,” Alder said, adding that if Utahns don’t adhere to public health messaging now, “we have the risk of this getting out of hand ... and all that really hard work we did at the beginning of the pandemic in Utah getting lost.”
“We’ve been ahead of it and now, we risk losing all of that,” he said.
Wearing a mask or face covering, Alder said, is not something that is easy or convenient for people, himself included.
“But given the alternative, they’re worth the effort,” he said.
Utah Gov. Gary Herbert has not yet mandated face masks statewide, relying instead on the hope that Utahns will “do the right thing,” as he has repeatedly said. He has, however, made them mandatory in state facilities and offices.
And individual health jurisdictions throughout the state have the ability to request to make masks mandatory should the data support it.
Higher case counts and widespread community transmission has warranted the requirement of face masks in public throughout Summit, Salt Lake and Grand counties and the city of Springdale, too. Health officials in each of those locations have sought and received approval to make face masks mandatory to further protect the public and dampen transmission.
U. physicians and researchers released a public service announcement on YouTube on Wednesday encouraging Utahns to wear masks.
“Do it for your kids, do it for your partner, do it for your mother, do it for your friend’s mother, do it for your neighbor, do it for all of us,” Dr. Andy Pavia, chief of pediatric infectious disease at University of Utah Health, said. “If we want to beat this, everyone has to wear a mask.”
Data from the antibody study shows that infections remained low when citizens of Utah were asked to “stay safe, stay home,” but then surged when those restrictions gradually lifted.
Related:
The option for larger gatherings and more freedom to move about in society led to more compromising situations, and because of the challenging nature of the virus that can be found even in asymptomatic people, the result was further spread. Officials strongly encouraged the use of face coverings, but not all people adhered.
Even with rising numbers, people still aren’t wearing masks.
“If we like to be able to function in ways that would get us back to normal or as close to normal as possible, we’ve got to adopt these precautions,” Alder said. “We just simply cannot stay in lockdown.”
Limiting crowds, maintaining physical distancing, staying home when sick, washing hands and following other guidelines pertinent to where we live, he said, will “help us see a post-COVID-19 world as soon as possible.”
As it stands, the study shows that Utah is doing better than most other locations in the U.S., with one of the lowest death rates among positive cases in the country, at about 1%.
Alder is hoping the surge in cases is just a “rough patch” and something the state can quickly correct.
“We’ve got a really good set of individuals and institutions helping us in our state,” he said. “Combined with the public being cooperative, we could have the best possible outcomes ... but we need the public to adhere to the recommended health guidelines.”